Extracorporeal Shock Wave Treatment
Sanuwave
An Overview
The benefits of extracorporeal shock wave treatment (ESWT) are broad and profound. ESWT can be effectively used in conjunction with other therapies to address acute and chronic soft tissue wounds. ESWT seems to work along many different pathways to facilitate healthy and complete healing. Among the benefits of ESWT are:
- an increase in blood flow perfusion
- epithelialization (reepithelialization) – covering the injury with new skin and mucous membranes
- facilitation of wound closure
- improved angiogenesis – formation of new blood vessels and capillaries
- improved tissue granulation – the filling of the wounds
- reduced necrotic fibrin tissue – dead tissue
- reduction in duration of healing
- reduction in the need for antibiotic use

Orthopedics Treatment
Musculoskeletal injuries are among the most common reasons for visiting a physician in the United States. More than 25% of Americans suffer from one kind of musculoskeletal impairment or another. This accounts for over 130 million doctor’s visits and $850 billion yearly. There is research currently underway examining the effectiveness of ESWT on these types of injuries. If successful, shock wave therapy could be added to the arsenal of effective, non-invasive treatments at physican’s disposal.
Non-Union Fractures
The United States medical field treats millions of broken bones a year. Of these, over one million require surgery. In order to prevent the fractures from healing improperly, the bone is physically rejoined. During the internal fixation procedure, as it is known, the surgeon will use special screws, plates, rods, wires, or nails to hold the bones in the correct place. The majority of all traumatic long bone fractures undergo surgery and internal fixation. With that said, fractures resulting from car accidents or other high-impact traumatic injuries remain at risk for poor healing. Between 10 to 30 percent of such fractures are at risk improper healing, including those that don’t correctly mend. Non-union joints lead to increased risks and complications.
Osteoporosis and Osteoarthritis
There are currently over 135 million people diagnosed with arthritis all over the world. This includes close to 33 million people over the age of 18 with osteoarthritis in the United States. The number of people suffering from osteoarthritis in the U.S. is expected to more than double in the next 10 years. One of the defining factors of osteoarthritis is the mechanical disintegration of cartilage and joint surfaces. Advanced cases of arthritis warrant surgery and joint replacement in up to 30 percent of patients. According to The American Joint Replacement Registry (AJRR) there are over one million joint replacements per year in the U.S. costing over $15 billion annually This number is expected to grow by 85% by the year 2030.
I have a Special Health Condition. Is ESWT Right for Me?
Some pre-existing medical conditions could possibly complicate ESWT procedures. More research is needed to determine the effectiveness and safety of using ESWT with different underlying health concerns. Your healthcare provider will complete a full medical history and exam before proceeding with ESWT. A discussion about the pertinent information regarding how these and other health conditions might affect the outcome of an ESWT procedure will likely follow.
The following is a list of treatments and pre-existing medical conditions that may raise red flags for your provider:
- a cuff rupture when treating the shoulder,
- anatomical anomalies in the treatment area,
- malignancies found in the treatment area,
- patients with coagulation disorders and
- the presence of inflammation in the treatment area
Additionally, treatment in the following areas has not yet been proven to be safe:
- in the area of the gonads
- in the lung area,
- on the spinal column and
- the head area.
There has been little to no research on ESWT in treating:
- children,
- individuals with implants in the treatment area,
- patients with pacemakers or
- pregnant women
Product Overview
The dermaPACE System is cleared by the U.S. Food and Drug Administration (FDA) for the treatment of diabetic foot ulcers. It is also CE Marked and for sale in select international markets.
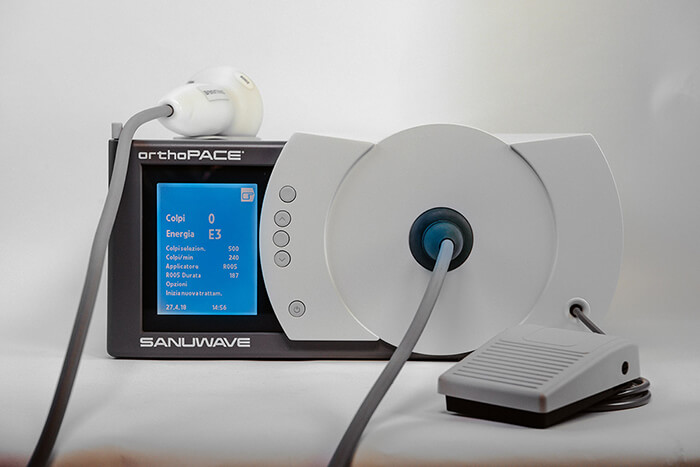
The orthoPACE System is CE Marked for international markets for orthopedic and musculoskeletal indications, but it is NOT CLEARED FOR USE in the United States by the U.S. Food and Drug Administration (FDA).
What About Safety?
Medical innovators originally designed Shockwave treatment to treat kidney stones back in the 1990’s. Over the interceding three decades, researchers and practitioners have collected a wealth of data and medical experience in the realm of Shockwave therapies. These practical lessons have been combined with advancements in engineering to produce a medical tool like none other on the market. The state-of-the-art dermaPACE device represents the gold standard in Shockwave technologies. Optimizing quality, efficacy and safety were at the heart of the development process. The dermaPACE has undergone comprehensive clinical studies and rigorous testing to confirm its safety and efficiency.
How long does it take to see results from Sanuwave treatments?
The timeline for seeing results from Sanuwave treatments can vary depending on the specific condition being treated and the individual patient. In some cases, patients may experience improvements shortly after the initial treatment, while in others, it may take several weeks or months to notice significant changes.
For conditions like chronic wounds or non-healing ulcers, it may take several weeks of regular Sanuwave treatments before visible improvements are observed. The treatment stimulates the body’s natural healing processes, which can take time to manifest in the form of wound closure, tissue regeneration, or improved circulation.
In musculoskeletal conditions, such as tendinopathies or orthopedic injuries, patients may start to experience pain reduction and improved mobility within a few weeks after starting Sanuwave treatments. However, it’s important to note that the full benefits and complete healing may take longer, and multiple treatment sessions may be required to achieve optimal results.
It’s crucial to consult with a healthcare professional who specializes in Sanuwave treatments to get a more accurate estimate of the expected timeline for results based on your specific condition and medical history. They can provide personalized guidance and monitor your progress throughout the treatment process.
It’s also worth noting that individual responses to Sanuwave treatments can vary, and some patients may respond more quickly or slowly than others. Factors such as the severity of the condition, overall health, and adherence to recommended treatment protocols can influence the speed and extent of the results.
Can Sanuwave be used for both acute and chronic conditions?
Yes, Sanuwave can be used for both acute and chronic conditions. Sanuwave’s technology is versatile and has applications in various medical fields, including wound healing, orthopedics, and pain management. It can be used to promote healing and pain relief in acute injuries or conditions, as well as in chronic conditions that require ongoing treatment and management.
How long do the results of Sanuwave treatment typically last?
The duration of results from Sanuwave treatment can vary depending on the specific condition being treated, the severity of the condition, and individual patient factors. In some cases, the results of Sanuwave treatment may be long-lasting, while in other cases, ongoing maintenance treatments may be required to sustain the benefits.
For example, in the case of musculoskeletal conditions such as chronic pain or orthopedic injuries, the results of Sanuwave treatment may be seen over a period of weeks to months. Improvement in pain levels, mobility, and functional outcomes may be observed after a series of Sanuwave treatments. However, the duration of the results can be influenced by factors such as the severity of the condition, the patient’s overall health, adherence to post-treatment recommendations, and other individual factors.
In the case of wound healing, Sanuwave has been shown to promote tissue regeneration and accelerate the healing process in chronic, non-healing wounds. The duration of results in wound healing can also vary depending on factors such as the size and depth of the wound, the patient’s overall health, and the presence of any underlying health conditions that may affect wound healing. In some cases, the results of Sanuwave treatment for wound healing may be long-lasting, while in other cases, ongoing maintenance treatments or wound care may be needed to sustain the benefits.
It’s Important to note that the results of Sanuwave treatment may also be influenced by individual patient factors, and outcomes can vary from person to person. It’s best to consult with a qualified healthcare professional who is experienced in using Sanuwave technology for a specific condition to get a better understanding of the expected duration of results based on your unique circumstances. They can provide personalized recommendations and follow-up care to help optimize the outcomes of Sanuwave treatment.
Are Sanuwave treatments suitable for all patients?
Sanuwave treatments are not necessarily suitable for all patients. They may not be recommended for individuals with certain conditions or health issues. For example, patients with active infections, cancer, or certain cardiovascular conditions might not be ideal candidates.
How does Sanuwave handle cases where patients experience adverse reactions to treatment?
Sanuwave addresses adverse reactions to its treatments through several key steps:
- Monitoring and Reporting: Healthcare providers are trained to monitor patients for any adverse reactions during and after treatment. Any issues are reported to Sanuwave for evaluation.
- Patient Assessment: If an adverse reaction occurs, the patient’s condition is assessed to determine whether it is related to the treatment or another factor.
- Adjustments or Discontinuation: Based on the assessment, adjustments to the treatment protocol may be made, or treatment may be discontinued if necessary.
- Medical Support: Patients experiencing adverse reactions are advised to seek medical attention to manage symptoms and address any complications.
- Review and Investigation: Sanuwave conducts a review of the reported adverse reactions to investigate the cause and make necessary adjustments to their protocols or device designs.
How does Sanuwave evaluate the suitability of treatments for patients with joint or bone conditions?
Sanuwave evaluates the suitability of treatments for patients with joint or bone conditions through several key steps:
- Medical Evaluation: Healthcare providers perform a thorough medical evaluation, including a review of the patient’s medical history, current condition, and any imaging or diagnostic tests, to determine if Sanuwave treatments are appropriate.
- Assessment of Condition: The specific nature and severity of the joint or bone condition are assessed. Sanuwave treatments are often used for conditions like chronic pain or delayed healing, but the suitability can vary depending on the individual case.
- Treatment Goals: The goals of treatment are discussed to ensure they align with what Sanuwave technology can effectively address.
Is it Safe for Everyone?
Medical professionals all over the world have come to believe that DermaPACE can facilitate proper and speedy healing in the vast majority of patients. It is, however, yet to be approved for use on patients with some special medical conditions. You should talk to your healthcare provider before undergoing DermaPACE therapy if you have any of the following medical conditions:
- coagulation disorders and
- malignancies in the treatment area.
PACE treatments have not been approved to be used on the following areas:
- the gonads,
- the area of the head,
- around the lungs and
- on the spinal column
There has had almost no experience in treating:
- children,
- individuals with implants in the treatment area,
- people with pacemakers or
- pregnant women.
Research conducted using Doppler imaging to measure blood flow in treatment areas have demonstrated a marked increase in blood perfusion and vessel density after 24 hours from treatment. This finding is valuable because it decreases the chances of ischemia (lack of blood flow) that is so often associated with inadequate healing. It is important to note that studies have shown that patients who have undergone PACE intervention did not experience any negative vascular side effects such as an unsafe change in blood pressure.
